November 23, 2021
Value-Based Critical Care
 As we look to the next phase of healthcare reform, there’s every reason to believe there will be a continued push on coverage expansion. Leadership from CMS (Centers for Medicare & Medicaid Services) and CMMI (Center for Medicare and Medicaid Innovation) are vocal about their commitment to payment policies that reward healthcare equity. We can also likely expect a continued push to migrate reimbursement models from fee-for-service to a value-based orientation. It’s becoming evident that CMS intends to move more aggressively to value-based payments around acute hospitalization and migrate the current voluntary bundled-payment program (Bundled Payments for Care Improvement Advanced) to a mandatory one as early as, or sooner than, 2023. Under mandatory bundles, hospitals across the country face a potential seven-figure risk.
As we look to the next phase of healthcare reform, there’s every reason to believe there will be a continued push on coverage expansion. Leadership from CMS (Centers for Medicare & Medicaid Services) and CMMI (Center for Medicare and Medicaid Innovation) are vocal about their commitment to payment policies that reward healthcare equity. We can also likely expect a continued push to migrate reimbursement models from fee-for-service to a value-based orientation. It’s becoming evident that CMS intends to move more aggressively to value-based payments around acute hospitalization and migrate the current voluntary bundled-payment program (Bundled Payments for Care Improvement Advanced) to a mandatory one as early as, or sooner than, 2023. Under mandatory bundles, hospitals across the country face a potential seven-figure risk.
To date, there has been more discussion on how hospital medicine and hospitalists can drive value-based care. However, this blog will highlight key points from our recent webinar, Value-Based Critical Care, and demonstrate how ICU care innovations and intensivists can improve quality and reduce costs to generate value and help hospitals succeed under value-based payment models.
INTENSIVE CARE IN THE US
Estimates state that at least five million patients are admitted to intensive care units yearly, usually through 70,000 adult ICU beds throughout the US. When we look at how this compares globally, it is interesting to find that when you look at the number of critical care beds per 100,000 habitants in any selected country and most of the advanced economies, the United States leads with 34.7 per 100,000 population. However, it’s important to emphasize that the US distribution might vary variable geographically depending on the concentration in large metros with more beds per 100,000 than more rural areas.
A 2016 study showed significant increases in the total ICU cost of care from $56.6 billion to $108 billion per year in the US between 2000 and 2010. In 2010, critical care medicine costs represented a little more than 4% of the national health expenditures. They represented .72% of the gross domestic product, which means that critical care is a high-acuity, high-cost area. While we don’t yet have updated data, there is no reason to believe that these numbers have not increased significantly in the last decade.
SIGNIFICANT OPPORTUNITIES FOR ICU IMPROVEMENTS
ICU Utilization
A study utilizing data from the Dartmouth Atlas shows significant variation in ICU admission rates regarding the number of patients admitted to an ICU based on 100 patients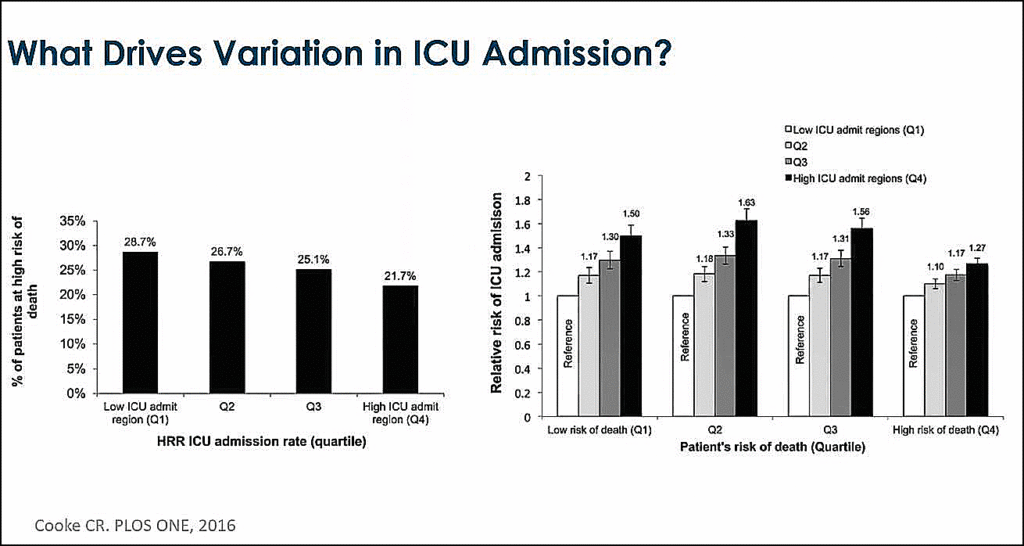 admitted to the hospital in that area. When identifying drivers of this variation, another significant study looked at quartiles related to the risk of death. And what you see (left chart) is the percent of patients at a high risk of death as measured by different severity scores that ended up in the ICU. It’s more likely that patient areas with lower ICU admittance rates will have a higher proportion of the highest risk patients. So, they admit fewer people to their ICUs, but they have a more significant proportion of patients at very high risk. However, the most interesting insight is that when you look at the relative risk of ICU admission compared to the patient risk of death in quartiles, you find the greatest variation lies in those gray zone patients with moderate and mild risk of death. This study illustrates a tremendous opportunity in standardizing who needs to go to the ICU.
admitted to the hospital in that area. When identifying drivers of this variation, another significant study looked at quartiles related to the risk of death. And what you see (left chart) is the percent of patients at a high risk of death as measured by different severity scores that ended up in the ICU. It’s more likely that patient areas with lower ICU admittance rates will have a higher proportion of the highest risk patients. So, they admit fewer people to their ICUs, but they have a more significant proportion of patients at very high risk. However, the most interesting insight is that when you look at the relative risk of ICU admission compared to the patient risk of death in quartiles, you find the greatest variation lies in those gray zone patients with moderate and mild risk of death. This study illustrates a tremendous opportunity in standardizing who needs to go to the ICU.
Other variations in ICU admissions can arise from regional differences, hospital infrastructure, types of diseases, or patients that present to an ICU. Several factors offer an opportunity for us to standardize and apply an evidence-based approach to decrease this variation of utilization and prevent overuse of the ICU as a resource.
Variations in Clinical Management
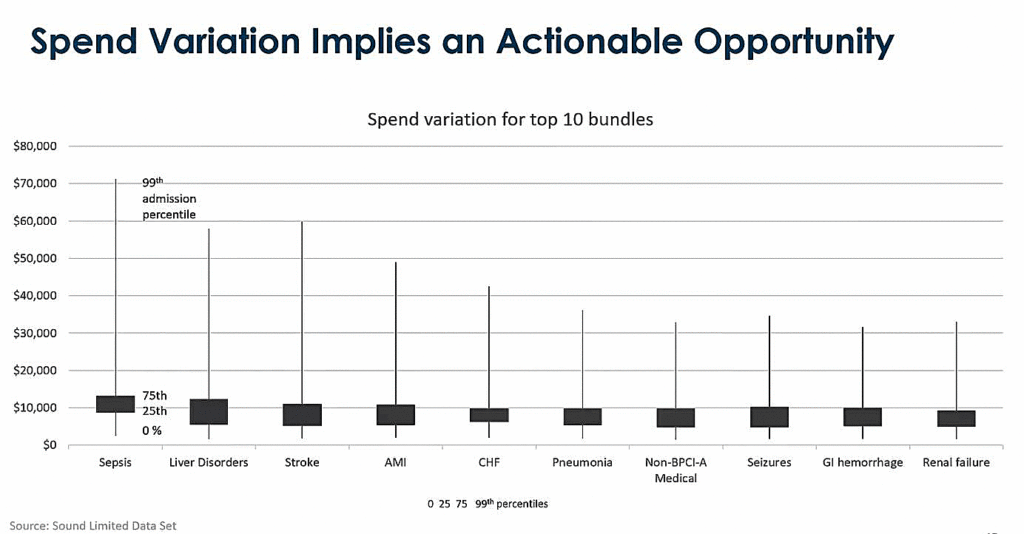 When we discuss variations in care and consider the top ten bundles of diseases, many of which diagnosis will end up in the ICU, it’s an easy insight to see a wide variation. The spend for sepsis per case, for example, can go from a few thousand to over $70,000 per admission, and what it implies is that there’s a tremendous opportunity to standardize how we treat these patients. There will always be a slight variation based on case details, but applying evidence-based care and standardizing the critical steps for each disease can help narrow that variation in spending and improve our ability to provide consistent quality.
When we discuss variations in care and consider the top ten bundles of diseases, many of which diagnosis will end up in the ICU, it’s an easy insight to see a wide variation. The spend for sepsis per case, for example, can go from a few thousand to over $70,000 per admission, and what it implies is that there’s a tremendous opportunity to standardize how we treat these patients. There will always be a slight variation based on case details, but applying evidence-based care and standardizing the critical steps for each disease can help narrow that variation in spending and improve our ability to provide consistent quality.
End-of-life Care
Statistics on healthcare spending for the last 12 months of life signal a further opportunity for critical care improvements. One Landmark study looked at the epidemiology of patients in the ICU at the end of their life and what they found is that as patients age, it is more likely they will be admitted to a hospital and or an ICU. The startling finding of this study was that one in five Americans die utilizing ICU services. This is a considerable number worth exploring. One could argue that this occurs because they are the sickest patients, but as we look closer, there could be a misalignment in goals based on patients’ wishes at the end of their life. There also might be a misalignment regarding what is evidence-based and most likely to benefit these patients. So again, this too demonstrates an opportunity to enhance how we manage end-of-life care in the ICU.
SOLUTIONS START WITH A HIGH-PERFORMING ICU
Before improvements in ICU utilization, variations in care, and end-of-life care, can be realized, the foundation of a high-performing ICU must be in place. Evidence-based practice in the ICU requires a structured, multidisciplinary approach involving intensivists, bedside nurses, and respiratory therapists working in cadence to develop evidence-based protocols. Protocols should be a living workflow and document that is updated regularly and adjusted, with compliance measures fed back to the bedside care team so that consistent practice is achieved and the team knows the “why” behind the evidence and how we intend to care for patients.
MDRs (multidisciplinary rounds) are indeed the cornerstone of a high-performing ICU program. MDRs should be a structured, consistent process involving all clinicians at the bedside. They should focus on communication across the team and measure performance management that ranges from individual provider performance to global metrics for patient outcome and efficiency.
Leadership development programs are also essential. When you’re a critical care fellow, they teach you to care for the sickest patients, but you don’t learn how to manage an ICU. Development should include education in ICU management, the economics behind care, the ability and techniques to manage other physicians, and the integration of an ICU program into the overall goals for patient care.
Development should include education in ICU management, the economics behind care, the ability and techniques to manage other physicians, and the integration of an ICU program into the overall goals for patient care.
On the technology front, Sound Physicians has successfully transformed its technology platform from just a charge/capture system to a platform for collecting structured performance data. Data will also provide nudges and reminders to clinicians on key care elements such as advanced care planning discussions and barriers to early hospital discharge.
Our telemedicine technology helps us build comprehensive critical care programs that use remote intensivists to address the shortage or maldistribution of intensivists. While we use ICU telemedicine for overnight coverage, we’ve also successfully provided virtual intensivists to conduct multidisciplinary rounds, coordinate care, and guide comprehensive critical care to all ICU patients.
With the proper foundation in place, critical care leaders are poised to deploy value-based care interventions to improve ICU utilization, variations in clinical practice, and end-of-life care. At Sound, we have also found that it’s essential for intensivists to have the authority and accountability for bed triage. Also, clinical integration with the hospital and emergency medicine teams play an important part.
To learn more detail about our value-based interventions and benefit from our recent webinar, please CLICK HERE.
